Evaluation of GPT-3.5 and GPT-4 for supporting real-world information needs in healthcare delivery
May 01, 2023Debadutta Dash, Rahul Thapa, Juan M. Banda, Akshay Swaminathan, Morgan Cheatham, Mehr Kashyap, Nikesh Kotecha, Jonathan H. Chen, Saurabh Gombar, Lance Downing, Rachel Pedreira, Ethan Goh, Angel Arnaout, Garret Kenn Morris, Honor Magon, Matthew P Lungren, Eric Horvitz, Nigam H. Shah
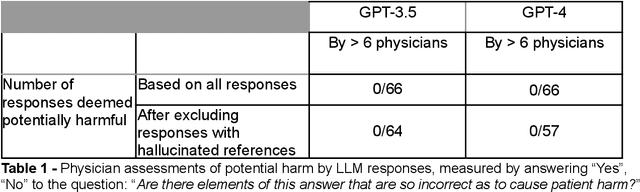
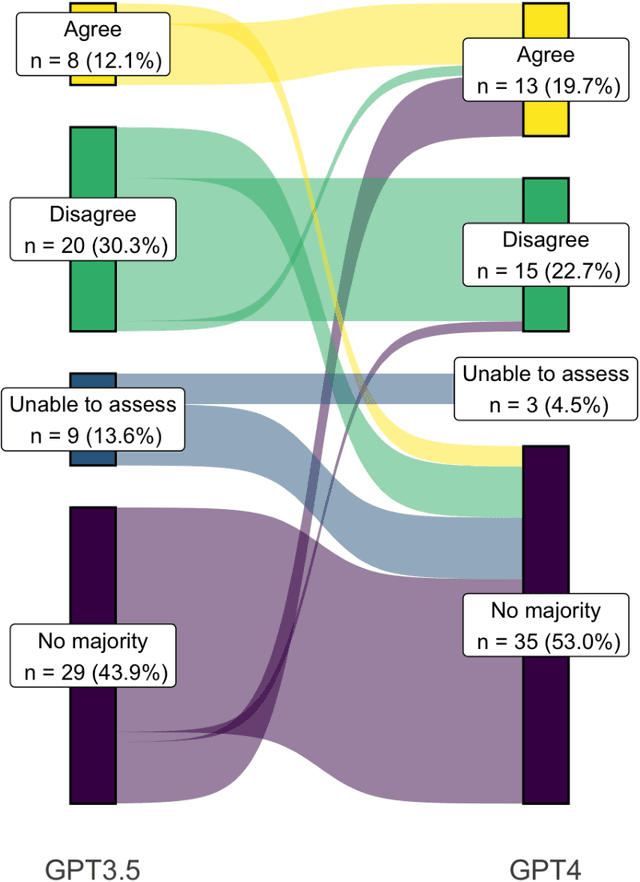
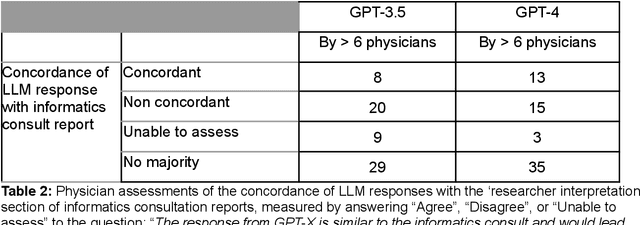
Despite growing interest in using large language models (LLMs) in healthcare, current explorations do not assess the real-world utility and safety of LLMs in clinical settings. Our objective was to determine whether two LLMs can serve information needs submitted by physicians as questions to an informatics consultation service in a safe and concordant manner. Sixty six questions from an informatics consult service were submitted to GPT-3.5 and GPT-4 via simple prompts. 12 physicians assessed the LLM responses' possibility of patient harm and concordance with existing reports from an informatics consultation service. Physician assessments were summarized based on majority vote. For no questions did a majority of physicians deem either LLM response as harmful. For GPT-3.5, responses to 8 questions were concordant with the informatics consult report, 20 discordant, and 9 were unable to be assessed. There were 29 responses with no majority on "Agree", "Disagree", and "Unable to assess". For GPT-4, responses to 13 questions were concordant, 15 discordant, and 3 were unable to be assessed. There were 35 responses with no majority. Responses from both LLMs were largely devoid of overt harm, but less than 20% of the responses agreed with an answer from an informatics consultation service, responses contained hallucinated references, and physicians were divided on what constitutes harm. These results suggest that while general purpose LLMs are able to provide safe and credible responses, they often do not meet the specific information need of a given question. A definitive evaluation of the usefulness of LLMs in healthcare settings will likely require additional research on prompt engineering, calibration, and custom-tailoring of general purpose models.
Missingness as Stability: Understanding the Structure of Missingness in Longitudinal EHR data and its Impact on Reinforcement Learning in Healthcare
Nov 16, 2019Scott L. Fleming, Kuhan Jeyapragasan, Tony Duan, Daisy Ding, Saurabh Gombar, Nigam Shah, Emma Brunskill

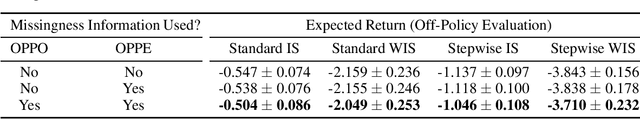
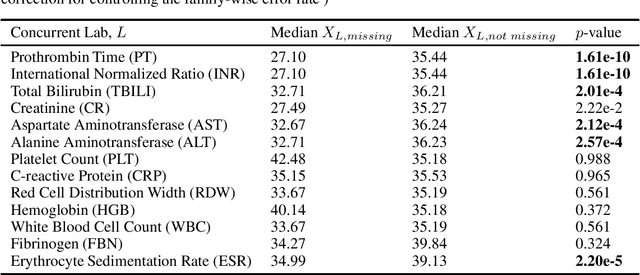
There is an emerging trend in the reinforcement learning for healthcare literature. In order to prepare longitudinal, irregularly sampled, clinical datasets for reinforcement learning algorithms, many researchers will resample the time series data to short, regular intervals and use last-observation-carried-forward (LOCF) imputation to fill in these gaps. Typically, they will not maintain any explicit information about which values were imputed. In this work, we (1) call attention to this practice and discuss its potential implications; (2) propose an alternative representation of the patient state that addresses some of these issues; and (3) demonstrate in a novel but representative clinical dataset that our alternative representation yields consistently better results for achieving optimal control, as measured by off-policy policy evaluation, compared to representations that do not incorporate missingness information.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge